What are floaters and flashes and why are they important?
Retinal Tears, Vitreous Detachment and Floaters PDF
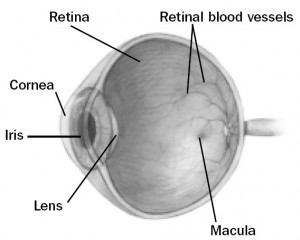
To help understand this question it is important to first understand the anatomy of the eye. The inside of the eye is filled with a gel like substance called the vitreous. The vitreous has a jello or egg-white consistency when we are young, and is firmly attached to the front of the eye on the inside (called the vitreous base). The retina is the very thin tissue that lines the inside of the eye cavity like wallpaper. When we look at something, the retina acts like the film in a camera and captures the image. The retina is attached to the wall of the eye only at the very front and at the back of the eye where the optic nerve goes to the brain. The vitreous is more lightly attached to the rest of the retina. Over time, the vitreous gradually becomes thinner and more liquid. It eventually collapses (analogy like a collapsed spider web), and separates from the retina. This separation of the vitreous from the retina is called a posterior vitreous detachment (PVD). PVD’s are typically harmless and cause increased floaters in the eye. In some cases however the traction on the retina may create a tear. Retinal tears frequently lead to retinal detachments as fluids seeps underneath the retina, causing it to separate and detach from the outer layers of the eye.
Are all floaters a sign of a problem?
No. Many people experience floaters when they are young and without having a PVD. These floaters are just condensations of the protein gel in the eye. They float in the cavity of the eye and cast tiny shadows on the retina. Floaters are more likely to develop as we age and are more common in people who are very nearsighted, have diabetes, or who have had a cataract operation. There are other, more serious causes of floaters, including infection, inflammation (uveitis), hemorrhaging, retinal tears, and injury to the eye. In most cases, floaters are part of the natural aging process and simply an annoyance. They can be distracting at first, but eventually tend to “settle” at the bottom of the eye, becoming less bothersome. They usually settle below the line of sight and do not go away completely. Most people have floaters and learn to ignore them; they are usually not noticed until they become numerous or more prominent. Floaters can become apparent when looking at something bright, such as white paper or a blue sky.
For people who have floaters that are simply annoying, no treatment is recommended. Floaters can rarely be so dense and numerous that they significantly affect vision. Usually with time these will settle down and be acceptable. In very rare cases , a vitrectomy may be needed. A vitrectomy removes the vitreous gel, along with its floating debris, from the eye. The vitreous is replaced with a salt solution. Because the vitreous is mostly water, you will not notice any change between the salt solution and the original vitreous. Surgery is not recommended unless the floaters seriously interfere with vision.
How do you treat a retinal tear?
If you develop a retinal tear it should be treated with laser to create a scar adhesion between the retina and the outer layers of the eye. Laser uses light to create heat at the spot where it is focused. This heat burns the tissue which heals as a scar adhering the tissues together. The retinal function in the areas of the laser is lost because the tissue is destroyed. Realize however that the area of the retinal tear is already not functioning as a result of the tear and that the tiny blind spot caused by the laser is only minimally larger. The laser treatment helps to prevent a subsequent retinal detachment in the vast majority of cases.
What do I watch out for after laser treatment of my retinal tear?
Any sudden increase in new floaters again could signify another tear and should be assessed. Also any loss of peripheral vision (like a shade or curtain being drawn from your peripheral vision toward the central vision) may be a sign of retinal detachment and needs to be assessed promptly. Call our office (780) 448-1801 with any of these changes.